The Three-Hit Model: Why APOE4 Alone Doesn’t Explain the Brain’s DHA Deficit
FADS genotype, APOE4 catabolism, and dietary linoleic acid may converge to create a progressive, age-dependent failure of brain DHA incorporation — and the data to test it already exist.
Jeannie Capone, BS, MSN, FNP-BC, PMHNP-BC
May 3, 2026
Part 2 of a series. Here is Part 1. if you missed it!
Abstract
Part 1 of this series critiqued the Andriambelo and Plourde (2026) study and proposed that the choroid plexus functions as a lipid triage center where DHA accumulates due to downstream resistance from n-6 long-chain species occupying neuronal membrane sn-2 positions. This second installment asks the upstream question: why is there a DHA deficit to triage in the first place? The answer, this article argues, is not a single gene — it is a three-hit convergence.
This article presents a mechanistic model and hypothesis derived from existing literature and is intended for scientific discussion and education. It is not medical advice and is not a substitute for individualized clinical care.
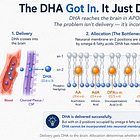
FADS genotype determines how much DHA the liver can synthesize from dietary precursors, with the low-converter TT genotype (rs174537) associated with substantially lower desaturase activity and reduced circulating long-chain PUFA levels compared to the high-converter GG genotype. Hit 2: APOE4 accelerates DHA catabolism (77% lower whole-body half-life), sequesters DHA in the liver, and impairs BBB transport (24% lower brain uptake). Hit 3: Dietary linoleic acid provides continuous substrate for AA and its elongation products (adrenic acid, DPA-n6), which occupy the neuronal plasmalogen sn-2 positions that DHA needs. No single hit is sufficient. But when all three converge — as they do in a postmenopausal European-ancestry woman carrying APOE ε4 and the TT FADS genotype on a high-LA Western diet — the result may be a progressive, age-dependent failure of DHA to reach its structural destination in the neuronal membrane. This model generates testable predictions using existing data from the ROSMAP cohort and may contribute to explaining the most puzzling observation in AD genetics: the incomplete penetrance of APOE4.
The Smoking Gun: Plasmalogen DHA and Cognitive Preservation
Before constructing the three-hit model, it is necessary to establish what is at stake — what, exactly, DHA does in the brain that makes its absence so consequential.
Goodenowe and Senanayake (2022) analyzed postmortem inferior temporal cortex tissue from 100 elderly subjects in the Rush Memory and Aging Project (MAP) and found that plasmalogen levels — specifically DHA-containing ethanolamine plasmalogens (PlsEtn 18:0/22:6) — were strongly and independently associated with cognitive function (β = 0.506, p < 0.00001 in multivariate analysis), even after accounting for amyloid plaque density, tau tangle burden, flotillin, and other measured neuropathological variables. The effect was dose-dependent. Subjects in the highest tertile of brain plasmalogen DHA maintained cognitive function even in the presence of substantial amyloid and tau pathology — the biochemical signature of cognitive resilience.
Mares et al. (2024) then examined brain and serum lipidomic profiles from the same cohort and found that APOE ε4 carriers with mild cognitive impairment showed lipidomic shifts consistent with altered Lands cycle acyl-chain remodeling: increased AA-containing phospholipids and decreased DHA-containing phospholipids in brain tissue. This pattern is consistent with the LPCAT3-mediated sn-2 competition model proposed in Part 1 — though Mares et al. did not directly test that mechanism. The Lands cycle — the deacylation/reacylation cycle that continuously remodels the sn-2 position of membrane phospholipids — was operating in APOE4 brains, but the balance of its substrates appeared shifted toward AA at the expense of DHA.
Together, these two studies from the same cohort establish that: (1) plasmalogen DHA at sn-2 is among the most important lipid variables for cognitive preservation, (2) the Lands cycle is the mechanism that determines what occupies sn-2, and (3) APOE4 brains show a Lands cycle shifted toward AA at the expense of DHA. The question becomes: what determines whether the Lands cycle installs DHA or AA at sn-2?
The answer requires looking upstream — at the three variables that together determine how much DHA is available to compete for sn-2 positions in neuronal plasmalogens.
Hit 1: FADS Genotype — The Liver’s DHA Manufacturing Capacity
The FADS gene cluster on chromosome 11q12.2 encodes the rate-limiting desaturase enzymes (Δ5-desaturase/FADS1 and Δ6-desaturase/FADS2) required to convert dietary alpha-linolenic acid (ALA, 18:3n-3) to EPA and ultimately to DHA. The common SNP rs174537 (G>T) tags a haplotype that determines FADS1 enzymatic activity, and its effect on circulating PUFA levels is among the largest of any common genetic variant: the TT genotype is associated with substantially lower desaturase activity and reduced circulating long-chain PUFA levels — including EPA and DHA — compared to GG carriers (Koletzko 2019). The magnitude of this effect on desaturase activity indices is large (often reported as 40–60% differences in product-to-precursor ratios), though the downstream impact on DHA specifically is attenuated because DHA sits at the end of a long conversion chain (ALA → SDA → ETA → EPA → DPA-n3 → DHA).
The allele frequency distribution is striking and directly relevant to AD epidemiology. In populations of European ancestry, the minor allele (T, low-converter) frequency is approximately 33%, yielding roughly 43% GG, 46% GT, and 11% TT. In populations of African ancestry, the derived allele (G, high-converter) frequency exceeds 95%, meaning approximately 81% are GG homozygotes with maximal FADS activity (Visioli 2026, Koletzko 2019). This creates a population-level asymmetry: European-ancestry individuals are far more likely to carry a genotype that limits endogenous long-chain PUFA synthesis.
Sasaki et al. (2019) provided the critical aging dimension. Using uniformly ¹³C-labeled linoleic acid in healthy young (25–34) versus elderly (65–74) participants, they showed that among FADS1 C allele carriers (the low-converter genotype), LCPUFA biosynthetic capacity was 32% lower in the elderly compared to the young — the already-disadvantaged genotype gets worse with age (Sasaki 2019). This is not a static genetic risk factor; it is a progressive metabolic decline. Of all the data points in this article, the Sasaki isotope-tracer finding is among the hardest — it is a direct measurement of enzymatic conversion, not an inference from circulating levels.
Schuchardt et al. (2016) demonstrated the clinical relevance directly: in 111 patients with mild cognitive impairment, minor allele carriers of multiple FADS SNPs had higher precursor PUFAs (LA, ALA) and lower AA — consistent with reduced desaturase activity. The mean omega-3 index was 6.19%, and over 85% of MCI patients had an omega-3 index below 8% (Schuchardt 2016). The population most vulnerable to cognitive decline is also the population with the lowest DHA synthesis capacity.
Hit 2: APOE4 — The Transport and Catabolism Deficit
The Plourde group’s body of work, reviewed in Part 1, has established that APOE4 creates a multi-level DHA deficit:
- Accelerated catabolism: Chouinard-Watkins et al. (2013) showed that APOE4 carriers have a 77% lower whole-body half-life of ¹³C-DHA, with the slope of the relationship between plasma DHA and β-oxidation 117% steeper — meaning APOE4 carriers burn DHA faster per unit of circulating DHA.
- Hepatic sequestration: Chouinard-Watkins et al. (2016) demonstrated that APOE4 mice have 60–100% higher liver AA, DHA, and FABP1 than APOE3 mice on control diet — the liver traps DHA rather than releasing it to plasma.
- Lower plasma availability: Husain et al. (2023) showed 20–30% lower plasma DHA in APOE4 mice independent of diet, and that APOE4 mice rely more on plasma DHA for cognitive function than APOE3 mice.
- Impaired BBB transport: Vandal et al. (2014) demonstrated that brain uptake of ¹⁴C-DHA is 24% lower in APOE4 versus APOE2 mice.
- Age-dependent Mfsd2a decline: Iwao et al. (2023) showed that 12- and 24-month-old mice had significantly reduced brain uptake of ¹⁴C-DHA and decreased Mfsd2a protein expression in brain microvasculature compared to 2-month-old mice (Iwao 2023). This age-related decline in the primary DHA transporter compounds the APOE4-specific transport deficit.
Each of these deficits is independently documented. Together, they mean that an APOE4 carrier starts with less DHA in plasma, loses it faster to β-oxidation, traps what remains in the liver, and transports less of what survives across the BBB — and all of these deficits worsen with age.
Hit 3: Dietary Linoleic Acid — The Substrate That Feeds the Competition
The third hit is the one that is entirely modifiable — and largely unaddressed in current APOE4 frameworks.
Linoleic acid (LA, 18:2n-6) is the dominant polyunsaturated fatty acid in the Western diet, comprising 7–10% of total energy intake — a 2–3-fold increase over evolutionary estimates. LA is the obligate precursor for AA (via FADS1/FADS2-mediated desaturation and elongation), and AA is the obligate precursor for adrenic acid (AdA, 22:4n-6, via ELOVL2/5-mediated elongation) and DPA-n6 (22:5n-6, via further desaturation).
As established in Part 1, these n-6 long-chain species — AA, AdA, and DPA-n6 — are the occupants of the neuronal plasmalogen sn-2 positions that DHA needs. The LPCAT3 crystal structure (Zhang 2021) shows structural preference for AA at sn-2. The cPLA2α/LPCAT3 cycle is self-reinforcing. AdA has turnover kinetics in brain plasmalogens equal to or slower than DHA (Masuzawa 1984), creating a hysteresis effect. And DHA incorporation into neural membranes is dependent on plasmalogen availability — if plasmalogen sn-2 positions are occupied by AdA, DHA may be less likely to be retained in neuronal phospholipids (Gaposchkin and Zoeller 1999).
Dietary LA is the upstream fuel for this entire competitive dynamic. Every molecule of LA that enters the FADS pathway can become AA, and every molecule of AA that is elongated becomes AdA — a particularly persistent occupant of the very plasmalogen positions that DHA requires. Reducing LA intake reduces the substrate pressure for AA/AdA production, potentially opening sn-2 positions for DHA. But no current APOE4 supplementation trial has tested DHA supplementation combined with LA restriction.
The sardine study by Díaz-Rizzolo et al. (2021) provides indirect support: one year of sardine supplementation (200g/week) in elderly prediabetic subjects decreased five omega-6 fatty acid species in erythrocyte membranes — including arachidonic acid and adrenic acid (both p 0.001) — while simultaneously increasing three omega-3 species (EPA, DPA-n3, DHA; all p 0.001). The omega-3 index increased from 6.64 to 7.90 in the sardine group. Critically, the sardine intervention replaced other dietary fats, effectively reducing LA intake while increasing preformed EPA and DHA — a dual intervention that the Andriambelo mouse study did not attempt.
The Three Hits Converge: A Multiplicative, Not Additive, Model
The three hits do not simply add up. They multiply.
Hit 1 alone (low FADS activity) is compensable: dietary preformed DHA bypasses the need for endogenous synthesis entirely. Populations with high fish intake and low FADS activity maintain adequate brain DHA.
Hit 2 alone (APOE4) is compensable: APOE4 carriers with high DHA intake and efficient FADS machinery can maintain adequate plasma and brain DHA. The Plourde group showed that 8 months of DHA-rich feeding abolished the hepatic sequestration difference between APOE3 and APOE4 mice (Chouinard-Watkins 2016).
Hit 3 alone (high LA intake) is compensable: if DHA supply is adequate, the Lands cycle can gradually displace AA and AdA from sn-2 through substrate pressure, one remodeling cycle at a time.
But when all three hits converge:
- Low FADS activity means endogenous DHA synthesis is impaired → the individual is dependent on dietary preformed DHA
- APOE4 means whatever DHA is consumed is catabolized faster, trapped in the liver, and transported less efficiently to the brain
- High LA intake means the neuronal membrane sn-2 positions are continuously resupplied with AA and AdA, maintaining the competitive disadvantage that reduces DHA incorporation even when it arrives
The result is a progressive, self-reinforcing deficit: less DHA arrives → less DHA competes for sn-2 → more AA/AdA remains at sn-2 → the Lands cycle maintains the n-6-dominant state → the brain’s plasmalogen DHA content declines → cognitive function declines.
The Three Hits Are Not Static — They Compound Across the Lifespan
The three-hit model describes a snapshot. But each hit worsens with age, creating a progressive narrowing of the window through which DHA can reach brain plasmalogens.
Hit 1 declines across three timescales. First, FADS activity itself decreases with aging — Sasaki et al. (2019) showed 32% lower LCPUFA biosynthetic capacity in elderly low-converter genotype carriers (Sasaki 2019). Second, ALA-to-DHA conversion is most efficient in childhood and declines through adulthood, meaning endogenous DHA supply naturally diminishes even before any genotype effect is considered. Third, menopause removes hormonal support for DHA synthesis. In HepG2 cells, progesterone upregulates FADS2 transcription — the rate-limiting step for ALA → DHA conversion — and this effect operates via epigenetic modification (hypomethylation of specific CpG loci in the FADS2 promoter); in human primary hepatocytes, the clearest effect was on FADS2 specifically rather than the full enzyme chain (Sibbons 2014). In ovariectomized rats, estradiol independently increases Δ6-desaturase protein expression and raises hepatic and plasma phospholipid DHA by 34–74% (Kitson 2013) — animal data that, while not direct postmenopausal human proof, is directionally consistent with the clinical observation from the Women’s Health Initiative: hormone therapy increased RBC DHA by 11% in 1,170 postmenopausal women aged 65–79, while simultaneously decreasing DPA-n3 by 10% — a pattern consistent with estrogen-induced upregulation of the final desaturation/elongation steps in the DHA synthesis pathway (Harris 2021). Both progesterone and estradiol decline precipitously at menopause.
Hit 2 also worsens with age independently of APOE genotype. Iwao et al. (2023) showed that 12- and 24-month-old mice had significantly reduced brain uptake of ¹⁴C-DHA and decreased Mfsd2a protein expression in brain microvasculature compared to 2-month-old mice (Iwao 2023). Even if DHA is synthesized and reaches plasma, its transport across the BBB declines with age.
Hit 3 — dietary LA — is the one variable that does not inherently worsen with age, but neither does it improve. Most individuals maintain the same high-LA Western dietary pattern throughout adulthood, meaning the substrate pressure for AA → AdA production remains constant while the DHA supply to counteract it progressively declines.
The convergence is striking: a postmenopausal woman with APOE4 and the TT FADS genotype on a high-LA Western diet faces the maximum possible version of all three hits — declining endogenous synthesis (age + FADS genotype + hormone loss), impaired transport (APOE4 + age-related Mfsd2a decline), and continuous AA/AdA substrate pressure (dietary LA). This is the highest-risk phenotype the model predicts.
The Ancestry Paradox: Why FADS Genotype May Contribute to Differential APOE4 Penetrance Across Populations
The following section is the most speculative component of the three-hit model. It is offered as a hypothesis-generating framework, not as an established explanation for observed epidemiological patterns.
The APOE ε4 allele frequency is highest in populations of African ancestry (~20–25%) and lowest in East Asian populations (~8–10%), with European populations intermediate (~13–15%). If APOE4 were the sole determinant of AD risk, African-ancestry populations should have the highest AD incidence. They do not — at least not proportionally to allele frequency. While AD incidence is higher in African Americans than European Americans, the per-allele risk conferred by APOE ε4 is substantially attenuated in African-ancestry populations compared to European-ancestry populations (Kaup 2015).
The three-hit model raises the possibility of a mechanistic contribution from FADS genotype. In populations of African ancestry, the FADS GG genotype frequency is approximately 81% — meaning the vast majority have maximal DHA synthesis capacity. Even with APOE4-mediated transport and catabolism deficits (Hit 2), the high FADS activity (Hit 1 is minimal) could partially compensate by maintaining higher peripheral DHA production. The per-allele impact of APOE4 may be partially buffered by efficient FADS machinery.
In populations of European ancestry, the TT genotype frequency is approximately 11% and the GT frequency is approximately 46% — meaning over half the population has suboptimal FADS activity. When APOE4 is layered onto a low-converter FADS genotype, both Hit 1 and Hit 2 are active simultaneously, and neither can compensate for the other. The per-allele impact of APOE4 may be amplified by inefficient FADS machinery.
This is a testable prediction, not an established fact. It generates a specific, falsifiable hypothesis: within APOE4 carriers, those with the GG FADS genotype should have later onset of cognitive decline and higher brain plasmalogen DHA than those with the TT genotype, after controlling for dietary DHA intake. Many other factors — socioeconomic, environmental, vascular, and genetic — also differ across ancestral populations and contribute to differential APOE4 penetrance. FADS genotype is proposed here as one potential contributor, not the sole explanation.
Why Some APOE4 Carriers Are Resilient: The FADS × Age Interaction as a Hidden Modifier
The Cache County Study (Khachaturian 2004) demonstrated that APOE ε4 primarily accelerates the age at onset of AD rather than determining lifetime susceptibility — the survival curves for 0, 1, and 2 ε4 alleles diverge in timing but converge at advanced ages, with a consistent proportion of individuals across all genotypes appearing resistant to AD. The question has always been: what distinguishes the resilient APOE4 carriers from the non-resilient ones?
The existing literature has focused on cognitive reserve, lifestyle factors, and a handful of genetic modifiers (KLOTHO-VS, CASP7, SERPINA3) (Huq 2019, Ferrari 2013). But to this author’s knowledge, no study has examined FADS genotype as a resilience modifier — despite the fact that it directly determines the substrate (DHA) that Goodenowe showed is strongly and independently associated with cognition in the Rush MAP cohort.
Freemantle et al. (2012) provided the critical bridge. They examined FADS1 haplotype variants in postmortem prefrontal cortex (BA47) from 61 male subjects aged 15–58 and found a significant interaction between FADS1 haplotype and age on brain fatty acid levels — specifically on estimated desaturase activity indices (Freemantle 2012). The minor haplotype (low-converter) was associated with altered fatty acid composition in brain tissue. But the critical finding was what they did not find: no difference in FADS1 or FADS2 mRNA expression in brain tissue between haplotypes. The brain is not making its own DHA differently based on FADS genotype — the brain FA composition differences are driven entirely by peripheral synthesis and transport.
This has a profound implication: the brain is a passive recipient of whatever DHA the liver sends it. If the liver’s FADS machinery is genetically impaired (TT genotype), hormonally depleted (menopause), and age-degraded (Sasaki 2019), the brain gets less DHA. No amount of local brain metabolism can compensate — at least not through the FADS pathway as expressed in brain parenchyma.
The age × haplotype interaction means the FADS effect on brain FA composition is not constant — it widens with age. Young adults with the minor haplotype may have brain FA profiles similar to major haplotype carriers (because peripheral DHA supply is still adequate from diet and residual FADS activity). But as aging compounds the FADS deficit, the gap widens. By age 58 (the oldest subjects in Freemantle’s cohort), the haplotype-dependent differences were measurable. Extrapolating to age 70–80 — the AD risk window — the gap would be expected to be substantially larger, though this extrapolation has not been directly tested.
The three-hit model predicts that resilient APOE4 carriers — those who remain cognitively intact past age 80 — should be enriched for the GG FADS genotype relative to non-resilient APOE4 carriers who developed AD at 65–75. The answer to APOE4 resilience may not be cognitive reserve or lifestyle alone. It may be that some APOE4 carriers were born with FADS machinery efficient enough to keep DHA in the plasmalogen seat for 80+ years despite the transport deficit — while others were not, and their brain plasmalogens slowly filled with AdA as their FADS capacity declined with age and hormonal loss.
Kaup et al. (2015) already showed that predictors of cognitive resilience differ by sex and race in APOE4 carriers — female sex was a predictor of resilience among Black APOE4 carriers but not White carriers (Kaup 2015). The three-hit model would predict this: Black women with APOE4 have the GG FADS genotype (81% frequency) potentially compensating for the APOE4 transport deficit, while White women with APOE4 are more likely to carry the TT genotype (no compensation) plus menopausal FADS decline.
The Contreras et al. (2026) GWAS of genetic modifiers of APOE4-associated cognitive decline identified loci linked to SEMA6D, GRIN3A, and ITGB8 — but notably, the FADS locus on chromosome 11 was not among the genome-wide significant hits (Contreras 2026). This could mean the FADS effect is mediated through lipid metabolism rather than direct cognitive pathways and would only be detected in a GWAS using brain lipidomic phenotypes rather than cognitive scores — meaning FADS genotype may modify APOE4 risk through a pathway (plasmalogen DHA content) that is invisible to cognitive GWAS but visible to lipidomic analysis.
The ROSMAP Opportunity: The Definitive Test Already Exists
The definitive test of the three-hit model may already be within reach. The ROSMAP cohort has genome-wide genotyping data imputed to the HRC reference panel, meaning rs174537 (the key FADS1 SNP) is almost certainly already available in the existing dataset — it is a common variant with MAF >25% in European populations that would easily pass standard imputation quality filters (Pérez-González 2024, Raghavan 2020). The Mares et al. (2024) Lands cycle lipidomics and the Goodenowe and Senanayake (2022) plasmalogen-cognition data were both generated from Rush Alzheimer’s Disease Center cohorts — Mares et al. using the combined ROSMAP dataset (dorsolateral prefrontal cortex) and Goodenowe using the Rush Memory and Aging Project subset (inferior temporal cortex). The shared infrastructure and harmonized protocols of these cohorts make cross-study integration feasible.The cohort also has longitudinal cognitive data, APOE genotyping, dietary records, and neuropathological staging.
Every variable needed to test the three-hit model exists in a single cohort. The analysis would be:
1. Extract rs174537 genotype from existing GWAS data
2. Stratify by APOE status (ε3/ε3 vs. ε3/ε4 vs. ε4/ε4)
3. Cross-reference with Goodenowe’s plasmalogen-specific sn-2 FA data (PlsEtn 18:0/22:6 vs. PlsEtn 18:0/22:4)
4. Test whether FADS genotype modifies the APOE4 effect on plasmalogen DHA content
5. Test whether the FADS × APOE4 interaction predicts cognitive trajectory independent of amyloid and tau
One important limitation: ROSMAP is approximately 97% non-Hispanic White, providing adequate power for the GG versus TT comparison within European ancestry but no power to test the African American FADS-mediated protection hypothesis. Testing that component would require a cohort with substantial African American enrollment and postmortem brain tissue — such as the Washington Heights-Inwood Columbia Aging Project (WHICAP) or the Minority Aging Research Study (MARS), also based at Rush.
A Cliffhanger: The Brain Blood Vessel as a Local DHA Factory
The three-hit model as described above assumes that brain DHA is entirely dependent on peripheral supply — hepatic synthesis plus dietary preformed DHA, transported across the BBB via Mfsd2a. Freemantle’s finding that brain FADS gene expression does not differ by genotype supports this assumption.
But Leikin-Frenkel et al. (2026) have just demonstrated something that may partially challenge it: brain blood vessel endothelial cells can locally synthesize DHA from ALA via the Δ6-desaturase pathway — and this local synthesis is suppressed when external DHA is provided (Leikin-Frenkel 2026). In female APOE4 mice, 6 months of an ALA-rich (flaxseed oil) diet restored brain parenchyma DHA levels, increased DHA-containing phospholipids, and improved memory — without providing any preformed DHA.
This finding, if confirmed, introduces a third source of brain DHA that may partially reduce reliance on Mfsd2a-mediated transport of circulating preformed DHA. But it also introduces a new dependency on FADS genotype: if the BBV endothelium’s Δ6-desaturase is encoded by the same FADS2 gene whose activity varies substantially by genotype (Visioli 2026), then the BBV’s local DHA synthesis capacity would be FADS-genotype-dependent — high in GG carriers, impaired in TT carriers. Whether this endothelial FADS2 activity is subject to the same genotype-dependent variation as hepatic FADS2 has not been directly tested.
The therapeutic implications are intriguing and will be explored in a future NeuroLipid Notebook article: for APOE4 carriers with high FADS activity, ALA-rich diets may be more effective than preformed DHA supplementation — because they could activate a local synthesis pathway that partially circumvents the very transport deficit that defines the APOE4 phenotype. For APOE4 carriers with low FADS activity, preformed DHA remains essential, but must be delivered at doses and durations sufficient to overcome the sn-2 competition described in Part 1. The optimal intervention may depend not on APOE status alone, but on the APOE × FADS interaction — a precision nutrition framework that no current clinical trial has tested.
Conclusion
The three-hit model — FADS genotype × APOE4 × dietary LA — reframes the APOE4-associated DHA deficit as a convergent, multiplicative, and age-dependent phenomenon rather than a single-gene transport problem. It raises the possibility that DHA supplementation trials have produced inconsistent results in part because they did not stratify by FADS genotype or control LA intake, that differential FADS allele frequencies across ancestral populations may contribute to the variable penetrance of APOE4, that menopausal FADS decline may be one factor in the disproportionate impact on women, and that some APOE4 carriers remain cognitively resilient because they carry FADS genotypes that maintain DHA supply despite the transport deficit.
The model is speculative but generates testable predictions that can be evaluated using existing data from the ROSMAP cohort — no new genotyping, no new tissue collection, no new clinical trial required. The experiment that could confirm or refute the central prediction (FADS genotype modifies the APOE4 effect on brain plasmalogen DHA) is already possible. Someone just needs to run it.
Part 3 will explore the therapeutic implications: ALA versus preformed DHA in the context of FADS genotype, the role of LA restriction as an adjunctive strategy, and the precision nutrition framework — APOE × FADS × sex × age — that should guide the next generation of intervention design.
PS. I have been building up to this point for some time. Here is another article that I think will be helpful as you approach this Series!
References
Goodenowe DB, Senanayake V. Relation of serum plasmalogens and APOE genotype to cognition and dementia in older persons in a cross-sectional study. Brain Sciences. 2019;9(4):92.
Goodenowe DB, Senanayake V. Brain ethanolamine phospholipids, neuropathology and cognition: a comparative post-mortem analysis of structurally specific plasmalogen and phosphatidyl species. Frontiers in Cell and Developmental Biology. 2022;10:866156
Mares J, Costa AP, Dartora WJ, et al. Brain and serum lipidomic profiles implicate Lands cycle acyl chain remodeling association with APOEε4 and mild cognitive impairment. Frontiers in Aging Neuroscience. 2024;16:1419253.
Koletzko B, Reischl E, Tanjung C, et al. FADS1 and FADS2 polymorphisms modulate fatty acid metabolism and dietary impact on health. Annual Review of Nutrition. 2019;39:21-44.
Visioli F, Alfredo Martínez J, Tomé-Carneiro J. Genetic modulation of omega-3 and omega-6 PUFA metabolism and health outcomes: a systematic review. Food & Function. 2026;17(5):2176-2191.
Sasaki H, Sueyasu T, Tokuda H, et al. Aging and FADS1 polymorphisms decrease the biosynthetic capacity of long-chain PUFAs: a human trial using [U-¹³C]linoleic acid. Prostaglandins, Leukotrienes, and Essential Fatty Acids. 2019;148:1-8.
Schuchardt JP, Köbe T, Witte V, et al. Genetic variants of the FADS gene cluster are associated with erythrocyte membrane LC PUFA levels in patients with mild cognitive impairment. Journal of Nutrition, Health & Aging. 2016;20(6):611-20.
Chouinard-Watkins R, Rioux-Perreault C, Fortier M, et al. Disturbance in uniformly ¹³C-labelled DHA metabolism in elderly human subjects carrying the apoE ε4 allele. British Journal of Nutrition. 2013;110(10):1751-1759.
Chouinard-Watkins R, Vandal M, Bhatt DK, et al. APOE4 genotype modulates hepatic DHA and AA concentrations in response to dietary supplementation. Prostaglandins, Leukotrienes and Essential Fatty Acids. 2016;112:7-13.
Husain MA, Laurent B, Bhatt DK, et al. APOE4 mice have lower plasma and brain DHA and AA, and higher hippocampal AA correlates with lower cognitive performance. Lipids in Health and Disease. 2023;22:67.
Vandal M, et al. Reduction in DHA transport to brain in apolipoprotein E4 targeted replacement mice. Journal of Neurochemistry. 2014;129(3):516-526.
Iwao T, Takata F, Matsumoto J, et al. Aging decreases docosahexaenoic acid transport across the blood-brain barrier in C57BL/6J mice. PLoS One. 2023;18(2):e0281946.
Zhang Q, Yao D, Rao B, et al. The structural basis for the phospholipid remodeling by lysophosphatidylcholine acyltransferase 3. Nature Communications. 2021;12(1):6869.
Masuzawa Y, Sugiura T, Ishima Y, Waku K. Turnover rates of molecular species of ethanolamine plasmalogens of rat brain. Journal of Neurochemistry. 1984;42(4):961-968.
Gaposchkin DP, Zoeller RA. Plasmalogen status influences docosahexaenoic acid levels in a macrophage cell line. Journal of Lipid Research. 1999;40(3):495-503.
Neu SC, Pa J, Kukull W, et al. Apolipoprotein E genotype and sex risk factors for Alzheimer disease: a meta-analysis. JAMA Neurology. 2017;74(10):1178-1189.
Sibbons CM, Brenna JT, Lawrence P, et al. Effect of sex hormones on n-3 polyunsaturated fatty acid biosynthesis in HepG2 cells and in human primary hepatocytes. Prostaglandins, Leukotrienes and Essential Fatty Acids. 2014;90(2-3):47-54.
Kitson AP, Smith TL, Bhatt DK, Bazinet RP. Influence of sex and ovariectomy on liver and brain DHA. Prostaglandins, Leukotrienes and Essential Fatty Acids. 2013;89(4):185-191.
Harris WS, Tintle NL, Sarter B, et al. Effect of hormone therapy on RBC omega-3 fatty acid content in postmenopausal women from the Women’s Health Initiative. Prostaglandins, Leukotrienes and Essential Fatty Acids. 2021;175:102362.
Kaup AR, Nettiksimmons J, LeBlanc ES, et al. Predictors of cognitive resilience to apolipoprotein E ε4 in diverse older women. Alzheimer’s & Dementia. 2015;11(7 Suppl):P556.
Freemantle E, Lalovic A, Bhatt DK, Mechawar N, Bhatt R, Bhatt DK, Bhatt R, Turecki G. Age and haplotype variations within FADS1 interact and associate with alterations in fatty acid composition in human male cortical brain tissue. PLoS One. 2012;7(8):e42696.
Contreras JA, et al. GWAS of genetic modifiers of APOE4-associated cognitive decline. 2026.
Leikin-Frenkel A, Ravid O, Liberman M, et al. α-Linolenic acid-rich diet boosts docosahexaenoic acid levels and restores lipid balance in the brain parenchyma and vasculature of APOE4 mice. Journal of Nutritional Biochemistry. 2026;154:110352.